NASH vs NAFLD: Key Differences in Liver Conditions Explained
Are you confused about liver disease terminology? Understanding the difference between NASH and NAFLD is crucial for anyone concerned about liver health. These conditions affect millions of people worldwide, yet many don't know they have them until significant liver damage has occurred. I've spent years researching these conditions and want to share what I've learned in simple terms.
When my uncle was diagnosed with a "fatty liver," our family was thrown into a world of confusing medical terminology. Was it NASH? Was it NAFLD? What did these acronyms even mean? If you're feeling similarly confused, you're not alone. This comprehensive guide will help clarify these two related but distinct liver conditions.
What is NAFLD (Non-Alcoholic Fatty Liver Disease)?
NAFLD, or Non-Alcoholic Fatty Liver Disease, is an umbrella term for a range of liver conditions that affect people who drink little to no alcohol. The defining characteristic is an excessive accumulation of fat in the liver cells. Think of NAFLD as the parent category that includes different stages of severity.
I remember talking with a hepatologist who explained NAFLD to me using a simple analogy: "Imagine your liver as a clean sponge. With NAFLD, that sponge slowly gets soaked with oil, but it can still function." This made it click for me - the liver is getting fatty, but it's not necessarily inflamed or damaged yet.
NAFLD has become increasingly common in recent decades, paralleling the rise in obesity, type 2 diabetes, and metabolic syndrome. In fact, it's now the most common form of liver disease in Western countries, affecting an estimated 25-30% of adults. What's particularly concerning is that many people have no idea they're affected - NAFLD often causes no obvious symptoms until the disease has progressed considerably.
One thing that surprised me during my research was learning that NAFLD isn't just a problem for older adults. Children can develop it too, especially if they're overweight or have certain metabolic conditions. I've even heard pediatricians discuss seeing more cases in their practices over the last decade. This really highlights how our modern lifestyles are affecting liver health across all age groups.
What is NASH (Non-Alcoholic Steatohepatitis)?
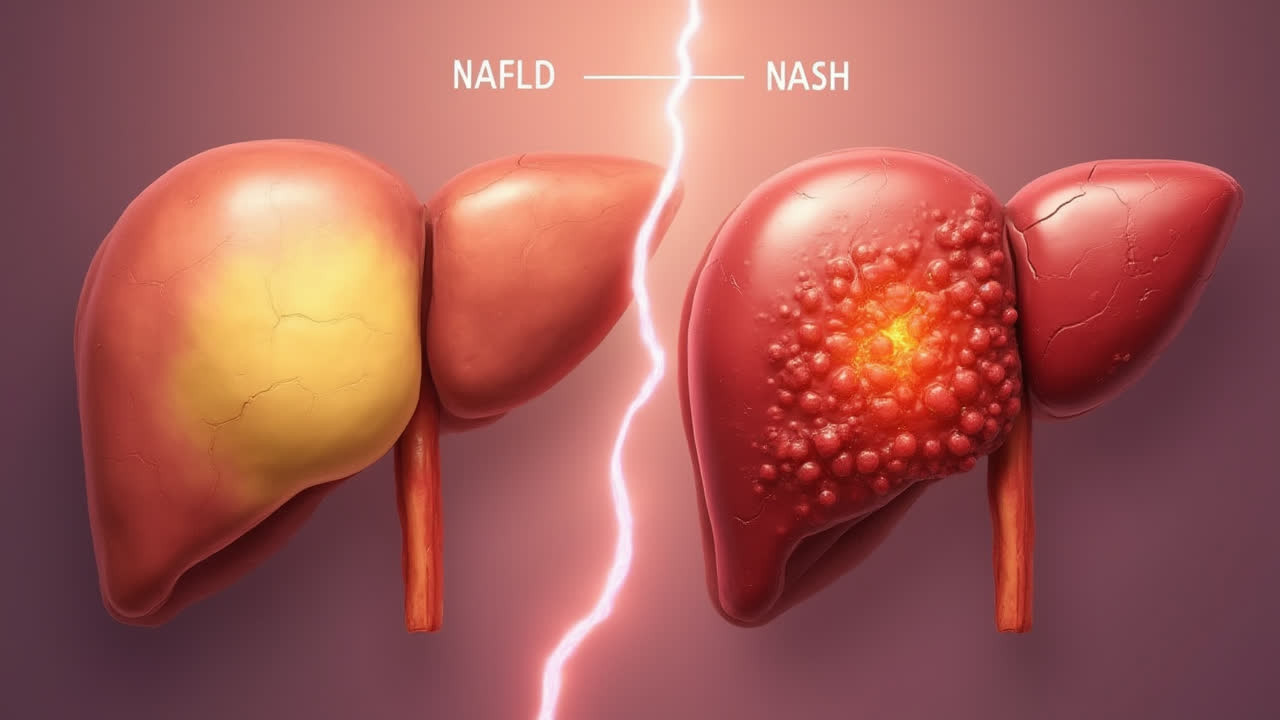
NASH, or Non-Alcoholic Steatohepatitis, represents a more serious form of NAFLD. The key difference is that NASH involves not just fat accumulation but also inflammation and liver cell damage. This inflammatory component is what makes NASH potentially progressive and dangerous.
Going back to our sponge analogy, with NASH, that oil-soaked sponge is now irritated, inflamed, and starting to deteriorate. The liver cells are under attack, and over time, scarring (fibrosis) can develop. If extensive scarring occurs, it can lead to cirrhosis, which is advanced liver scarring that can impair liver function and potentially lead to liver failure or cancer.
Approximately 20% of people with NAFLD will progress to develop NASH. This progression isn't fully understood, but researchers believe that multiple factors contribute, including genetic predisposition, gut health, and ongoing metabolic issues. I've spoken with patients who were shocked to learn their "simple fatty liver" had progressed to NASH without them experiencing any noticeable symptoms.
The silent nature of these conditions is perhaps their most dangerous aspect. By the time symptoms like fatigue, abdominal discomfort, or jaundice appear, significant liver damage may have already occurred. That's why understanding the distinction between NAFLD and NASH is so important - it helps emphasize the potential seriousness of what might otherwise be dismissed as "just a fatty liver."
NASH vs NAFLD: Understanding the Relationship
To clarify the relationship between these conditions: NAFLD is the broader category that encompasses different stages of fatty liver disease. Within NAFLD, there are two main types:
- NAFL (Non-Alcoholic Fatty Liver): Simple fatty liver without inflammation or cell damage
- NASH (Non-Alcoholic Steatohepatitis): Fatty liver with inflammation and cell damage
So all cases of NASH are by definition forms of NAFLD, but not all cases of NAFLD are NASH. It's a hierarchical relationship - NASH is essentially NAFLD that has progressed to a more serious stage.
I've found that visualizing this relationship helps tremendously in understanding these conditions. Imagine a pyramid where the base is NAFLD, and as you move up, you reach NASH, with cirrhosis at the very top. Not everyone will progress up this pyramid - many people with NAFLD will remain at the simple fatty liver stage without inflammation. But for those who do progress to NASH, the risk of further complications increases significantly.
What makes this distinction particularly important is that while simple fatty liver (NAFL) rarely leads to serious liver problems, NASH can progress to cirrhosis, liver failure, and even liver cancer. This progression isn't inevitable - with appropriate lifestyle changes and medical management, NASH can be controlled and sometimes even reversed. But the first step is proper diagnosis and understanding of which condition you're dealing with.
Comparative Analysis: NASH vs NAFLD
| Characteristic | NAFLD | NASH |
|---|---|---|
| Definition | Umbrella term for excess fat in the liver due to non-alcoholic causes | Specific subtype of NAFLD with inflammation and liver cell damage |
| Liver Changes | Fat accumulation only (in simple NAFL) | Fat accumulation plus inflammation and cell damage |
| Symptoms | Often asymptomatic; possibly fatigue and right upper abdominal discomfort | Similar to NAFLD but may include more pronounced fatigue, abdominal swelling, enlarged spleen, red palms, jaundice in advanced cases |
| Risk of Progression | Simple NAFL has low risk of progression to cirrhosis | Significantly higher risk of progression to cirrhosis, liver failure, or cancer |
| Prevalence | 25-30% of general adult population | 3-5% of general adult population (about 20% of NAFLD cases) |
| Diagnosis Method | Blood tests, imaging (ultrasound, CT, MRI) | Liver biopsy is the gold standard |
| Treatment Focus | Weight loss, management of metabolic conditions | Same as NAFLD plus specific treatments for inflammation and fibrosis |
| Monitoring Requirements | Regular but less frequent monitoring | More intensive monitoring for disease progression |
Causes and Risk Factors
Both NAFLD and NASH share similar risk factors, centered around metabolic health issues. The most common contributing factors include:
- Obesity, especially central (abdominal) obesity
- Type 2 diabetes or insulin resistance
- High blood lipids (cholesterol and triglycerides)
- Metabolic syndrome
- Rapid weight loss or poor nutrition
- Certain medications
- Genetic predisposition
The connection between these conditions and metabolic health is so strong that some experts have proposed renaming NAFLD to "Metabolic Associated Fatty Liver Disease" (MAFLD) to better reflect its relationship with metabolic dysfunction. I've noticed in my conversations with liver specialists that they often emphasize looking beyond the liver to address the underlying metabolic issues.
Interestingly, not everyone with these risk factors will develop NAFLD, and not everyone with NAFLD will progress to NASH. There seems to be a complex interplay between genetic susceptibility, gut microbiome health, dietary factors, and lifestyle influences. I remember attending a medical conference where researchers were discussing how two patients with identical BMIs and metabolic profiles could have vastly different liver outcomes - highlighting how much we still have to learn about individual susceptibility.
One particularly fascinating area of emerging research is the role of the gut-liver axis in these conditions. The gut microbiome (the collection of bacteria living in our intestines) appears to influence liver health significantly. Disruptions in the balance of gut bacteria may contribute to the inflammation that characterizes NASH. This connection makes perfect sense when you consider that everything absorbed from our intestines passes directly to the liver through the portal vein.
Diagnosis and Diagnostic Challenges
Diagnosing NAFLD and distinguishing it from NASH presents significant challenges. Many patients remain undiagnosed until the disease has progressed substantially. The typical diagnostic journey includes:
- Blood tests to assess liver function and rule out other causes of liver disease
- Imaging studies like ultrasound, CT scans, or MRI to detect fat in the liver
- Specialized tests like FibroScan (transient elastography) to assess liver stiffness
- Liver biopsy, which remains the gold standard for definitively diagnosing NASH and assessing the degree of inflammation and fibrosis
The reliance on liver biopsy for definitive NASH diagnosis is problematic due to its invasive nature, sampling error potential, and cost. This has driven intense research into non-invasive alternatives. I recently read about promising blood-based biomarkers and advanced imaging techniques that might eventually replace the need for biopsies in many patients.
Another challenge in diagnosis is that liver enzymes (ALT and AST), which are commonly used to screen for liver problems, can be normal in up to 80% of people with NAFLD. This means many cases go undetected during routine blood work. I've met several patients who were surprised to learn they had significant fatty liver disease despite having "normal" liver tests during their annual physicals.
The diagnostic uncertainty can be incredibly frustrating for patients. One woman I interviewed for a health article told me she spent nearly two years going from doctor to doctor, experiencing fatigue and vague abdominal discomfort, before finally being diagnosed with NASH. Her liver enzymes were only mildly elevated, which didn't trigger concern at first. Her story highlights the importance of considering liver health even when obvious red flags aren't present, especially in people with metabolic risk factors.
Treatment Approaches for NAFLD and NASH
The good news is that both NAFLD and NASH can be managed and potentially reversed, especially in earlier stages. Treatment strategies include:
Lifestyle Modifications - These form the cornerstone of treatment for both conditions:
- Weight loss through dietary changes and increased physical activity (a 7-10% reduction in body weight can significantly reduce liver fat and inflammation)
- Mediterranean diet or other plant-rich eating patterns low in processed foods
- Regular exercise (both aerobic and resistance training)
- Avoiding alcohol and potentially hepatotoxic medications
- Managing diabetes, high blood pressure, and high cholesterol
Medications - While no drugs are currently FDA-approved specifically for NAFLD or NASH, several medications may be prescribed to address underlying issues or are being investigated in clinical trials:
- Vitamin E (for non-diabetic NASH patients)
- Pioglitazone (for some patients with NASH and diabetes or prediabetes)
- GLP-1 receptor agonists (medications originally developed for diabetes that also promote weight loss)
- Various experimental drugs targeting different pathways in NASH development
I've been following the pharmaceutical developments in this space with great interest. The race to develop effective NASH medications has become one of the hottest areas in drug development, with dozens of compounds in various stages of clinical trials. Given the enormous number of people affected by these conditions, an effective NASH medication could potentially become one of the most widely prescribed drugs worldwide.
For advanced cases that have progressed to cirrhosis or liver failure, liver transplantation may become necessary. Unfortunately, I've seen how the growing prevalence of NAFLD-related liver failure is putting additional pressure on already scarce donor organs. This reinforces the importance of early intervention to prevent progression to these advanced stages.
Living with NAFLD or NASH: Long-term Outlook
The prognosis for people with NAFLD and NASH varies greatly depending on the stage of disease, presence of fibrosis, and response to lifestyle changes. For those with simple fatty liver without inflammation, the liver-related outlook is generally good, though these individuals remain at higher risk for cardiovascular disease due to shared risk factors.
For those with NASH, especially with fibrosis, the situation requires more careful monitoring and aggressive management. Studies suggest that NASH with advanced fibrosis can reduce life expectancy, primarily through increased risk of liver-related complications and cardiovascular events.
I've been encouraged by stories of successful management, though. One memorable case involved a middle-aged man diagnosed with early NASH who completely reversed his condition through a combination of Mediterranean diet, daily walking, and strength training twice weekly. Within 18 months, his follow-up tests showed resolution of liver fat and inflammation. His case isn't unique - research consistently shows that lifestyle interventions can be remarkably effective.
Beyond the medical management, living with these conditions involves emotional and psychological challenges. The invisible nature of liver disease can make it difficult for family and friends to understand the fatigue and other symptoms that may affect daily life. Support groups, both online and in-person, can provide valuable connections with others facing similar challenges.
FAQ About NASH and NAFLD
Yes, especially in earlier stages, both NAFLD and NASH can be reversed completely with appropriate lifestyle changes. Weight loss of 7-10% of body weight has been shown to resolve liver fat and inflammation in many patients. However, once significant fibrosis or cirrhosis has developed, the scarring may be permanent even if the active disease process is halted. This is why early detection and intervention are so important. Even in advanced cases, proper management can prevent further progression and reduce complications.
While liver biopsy remains the gold standard for diagnosing NASH, several non-invasive methods can help assess the likelihood of NASH and fibrosis. These include specialized blood test panels like the NAFLD Fibrosis Score, FIB-4 index, or Enhanced Liver Fibrosis (ELF) test; imaging studies like FibroScan (transient elastography) or MR elastography that measure liver stiffness; and newer multi-parametric MRI techniques that can detect inflammation. Your healthcare provider might use a combination of these approaches, along with risk factor assessment, to determine the likelihood of NASH without performing a biopsy. However, in cases where the diagnosis remains uncertain and would affect treatment decisions, a biopsy may still be recommended.
Research suggests that the Mediterranean diet has the strongest evidence for NAFLD and NASH management. This diet emphasizes olive oil, nuts, fruits, vegetables, whole grains, fish, and limited red meat. The Mediterranean approach helps reduce liver fat even without significant weight loss, though combining it with calorie reduction enhances benefits. Other beneficial approaches include limiting added sugars and refined carbohydrates, which can contribute to liver fat accumulation. Specifically, sugar-sweetened beverages and high-fructose corn syrup should be minimized, as fructose metabolism places particular strain on the liver. Intermittent fasting protocols are also showing promise in early research. The key principle is finding a sustainable eating pattern that promotes gradual weight loss while providing good nutrition, rather than following extreme short-term diets.
Conclusion
Understanding the difference between NASH and NAFLD is more than just a matter of medical terminology - it has important implications for risk assessment, monitoring, and treatment approaches. NAFLD represents a spectrum of conditions ranging from simple fatty liver to the more serious NASH with inflammation and potential progression to cirrhosis.
The rising prevalence of these conditions, driven largely by the global increase in obesity and metabolic syndrome, makes it increasingly likely that you or someone you know may be affected. The good news is that with proper understanding, early detection, and appropriate lifestyle changes, these conditions can often be managed successfully and even reversed.
As research continues to advance our understanding of these conditions, we can expect better diagnostic tools, more targeted treatments, and improved outcomes for patients. In the meantime, maintaining a healthy weight, eating a balanced diet rich in plants, staying physically active, and getting regular health check-ups remain the best strategies for protecting your liver health.
Have you been diagnosed with NAFLD or NASH? What approaches have helped you manage your condition? Sharing experiences can be invaluable for others on similar health journeys.